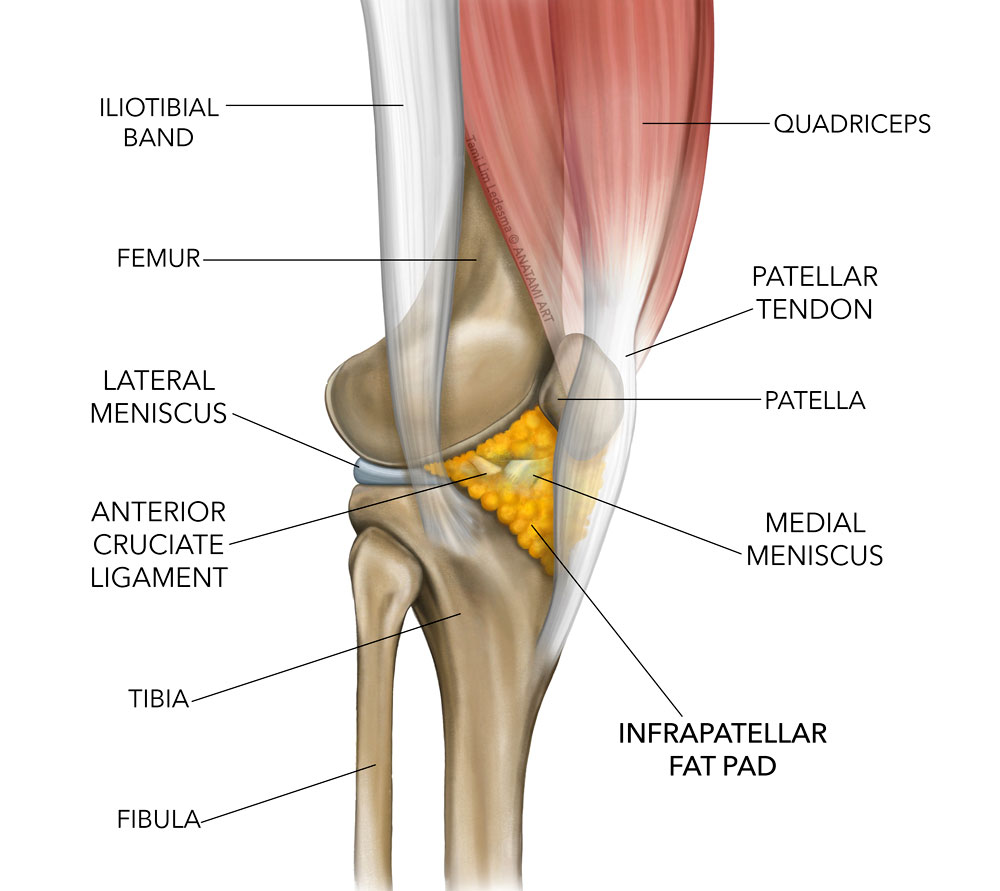
The Infrapatellar Fat Pad or Hoffa Pad (discovered by Albert Hoffa in 1904) is a soft tissue located under the patella and behind the patellar tendon. The infra-patellar fat pad is a shock absorber and protects the condyle (or end of the femur) in the event of a direct impact to the front of the knee. It also reduces friction between the patella, the saphenous nerve, and the skeletal structure of the knee.
Knee fat pads have a lot of nerve cells, so any damage to them is very painful. Acute or chronic inflammation of the infrapatellar fat pad is called fat pad syndrome or Hofa syndrome, a common cause of knee pain.
The prevalence of this disease in women is up to 3 times that of men, and the highest prevalence of the disease is in the age group of 40 to 60 years. Jumping exercises and ligamentous laxity are risk factors.
Causes of Infrapatellar Fat Pad Syndrome
Irritation and inflammation of the fat pad in the knee can be acute or chronic and can occur for the following reasons:
- Trauma to the front of the knee due to trauma or fall
- Excessive sports activity
- Anterior cruciate ligament (ACL) injury reduces knee stability and makes the infra-patellar fat pad more prone to injury.
- People with a history of knee hyperextension or genu recurvatum
- Stiffness of the quadriceps muscles
Knowing what the problem is can alleviate your worries
Symptoms of Infrapatal Fat Pad Syndrome
Symptoms of Infrapatellar Fat Pad Injury include:
- Pain, inflammation, and swelling in the front of the kneecap and on both sides of the patellar tendon
- Sensitivity to touch below and below the kneecap
- Increased pain in the extension (smoothing) of the knee
- Increased pain when standing for a long time
- Increased pain when squatting or going downstairs

Diagnosis of Infrapatellar Fat Pad Syndrome
- Physical examination and detailed examination of the knee by an orthopedic specialist
- Hoffa test: An evaluation method that involves moving the kneecap during quadriceps muscle contraction; in this test, the doctor asks the patient to lie on a bent knee (30 degrees), then gently straighten his leg while the doctor presses his fingers under the patella of the knee and on the lateral margin of both sides of the patellar tendon. Any pain or tenderness when straightening the foot is a positive test for Hofa syndrome.
- MRI: Used to assess the pathology of infra-patellar fat pad syndrome, including fibrosis, inflammation, and edema.
Treatments for Infrapatellar Fat Pad Syndrome
The goal of infrapatellar treatment is to reduce pain, improve knee strength, and prevent further injuries.
The doctor offers a specific treatment plan based on the mechanism of the injury. Since this complication is an inflammatory disease, non-surgical treatments are usually used to reduce inflammation, which includes the following:
Rest
Damaged tissues in the knee need time to heal. Rest prevents further damage and reduces pressure on tissues that are already inflamed. If the injury is severe, using a crutch or cane (which is placed in the opposite hand of the injured foot) can prevent excessive weight on the knee in the early days of the injury and when walking is essential.
Cold compresses
Applying ice is very useful to relieve acute symptoms and reduce inflammation (ice can be used for 10 minutes per hour). Ice helps to reduce pain in the front of the knee and prevents swelling and heat. The patient should apply ice immediately after injury to prevent possible inflammation as much as possible. This will help ensure a speedy recovery. Do not apply it directly to the skin. It is recommended that the patient examine the skin every 5 minutes to prevent burns from cold temperatures. All this should be placed in a damp towel and applied to the knee every 2 hours for approximately 15 minutes. Apply repeatedly during the first two days for two days.
- Placing the knee above the heart level helps control swelling by helping the body reabsorb fluid that has penetrated the tissue. If the patient cannot lie down (for example, at work), it is even helpful to place the knees on a chair.
- Compression
Use a bandage on the knee; this will help prevent inflammation and swelling. Tie the bandage from the middle of the thigh to the middle of the leg, make sure it is not too tight and open it at night.
Medication
Nonsteroidal anti-inflammatory drugs (NSAIDs) can help reduce pain, inflammation, and swelling. Mild painkillers can be helpful for the discomfort caused by pain in the front of the knee. Anti-inflammatory drugs can help reduce pain and swelling and get people back to work sooner.
Massage
If the swelling and pain in the front of the knee are severe, massage can help. While the foot is held in a high position, start the massage strokes from the knee to the thigh. This helps remove excess fluid from the knee tissue and return it to the bloodstream.
Physiotherapy
Physiotherapy is effective in managing anterior knee pain for a variety of reasons. One of the best ways to reduce pain and improve the function of an injured knee is to strengthen the hip and quadriceps, both of which protect the mechanics of the knee. By strengthening these areas properly, the patient can normalize the forces placed on the knee, assist in the healing process, and reduce the risk of recurrence of pain.
Electrotherapy
Electrotherapy uses electrical energy to stimulate the muscles and nerves inside the knee to create natural mechanisms for the treatment of various diseases, including pain in the front of the knee. This stimulation is believed to suppress interleukin-1 (IL-1), the cytokine responsible for regulating immune and inflammatory responses in the brain. It is also believed to release endorphins, stimulate the gray area of the brain, and act on pain receptors to reduce and possibly eliminate knee pain.
Electrotherapy methods that are recommended for the treatment of patients with anterior knee pain include ultrasound, electrical stimulation (TENs), magnet therapy and biofeedback electromyography.PRP
If the pain in the front of the knee persists, there has recently been a tendency to inject PRP to repair the patellar tendon. Platelet-rich plasma therapy is an alternative treatment in which the patient’s blood is used to repair damage by activating the body’s healing mechanism. In this method, the composition of the blood is reversed, and the healing properties of platelets are manipulated. This treatment is used to heal ligaments, tendons, muscles, and bone injuries. For PRP injection, the patient’s blood is taken and centrifuged to separate the various blood components. The plasma-containing layer is separated from the platelets, and the rest of the material is discarded. When this PRP is injected at the site of injury, these platelets are activated, releasing alpha granules that activate the patient’s growth factors and then stimulate epithelial growth factors (EGF). EGF induces cell migration and proliferation at the injury site and stimulates damaged tissue to heal.
Surgery
If knee pain does not respond to non-surgical treatments, your doctor may recommend knee surgery.
In some cases of patellar instability, in which the knee’s patella usually moves out of place, the doctor will usually have to perform surgery to repair the ligament that holds the patella in place. In cases of severe patellar osteoarthritis, if the patient does not respond to knee braces and physiotherapy, the doctor will sometimes need a joint replacement. Surgery, although rarely needed, can be very effective in severe cases of runners’ knees.





