Myofascial pain syndrome, MPS, is a common chronic pain disorder affecting various body parts. In skeletal muscles, MPS is characterized by hyperirritable spots called trigger points.
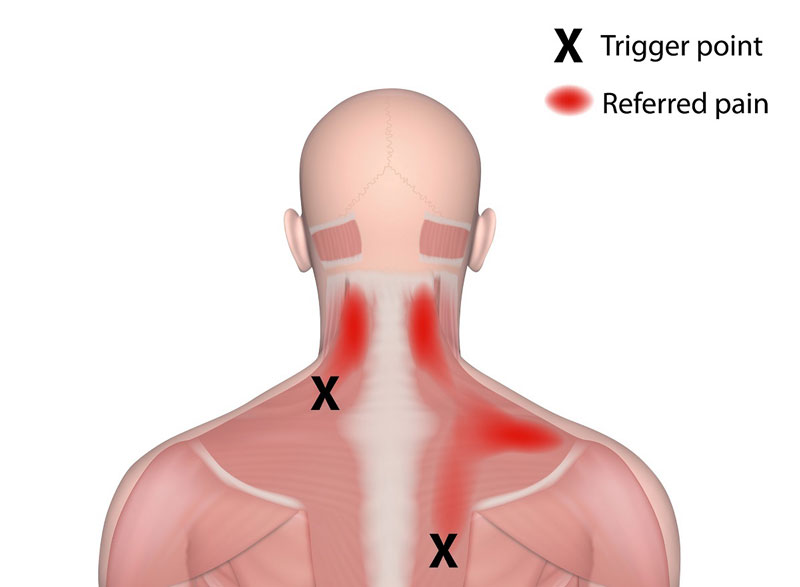
A trigger point can be felt as a band or a nodule of muscle with harder than normal consistency. Palpation of trigger points may elicit pain in a different area of the body. This is known as referred pain. Referred pain makes diagnosis difficult because the pain mimics symptoms of more well-known common conditions.
For example, trigger point-related pain in the head and neck region may be mistaken as tension headache, temporomandibular joint pain, eye pain, or tinnitus. Symptoms of MPS include regional, persistent pain commonly associated with a limited range of motion of the affected muscle.
The pain is most frequently found in the head, neck, shoulders, extremities, and lower back.
Trigger points are developed due to muscle injuries, which can be caused by acute trauma, such as sports injury, or chronic muscle overuse brought by repetitive activities, emotional stress or poor posture.
A trigger point comprises many contraction knots where individual muscle fibres contract and cannot relax. These fibres shorten the muscle and constitute a taut band – a group of tense muscle fibres extending from the trigger point to the muscle attachment.
The sustained contraction of these fibres compresses the local blood supply, resulting in an energy shortage in the area. This metabolic crisis activates pain receptors, generating a regional pain pattern that follows a specific nerve passage. The pain patterns are therefore consistent and are well documented for various muscles.
Causes of Muscle Pain?
Muscles can hurt for a variety of reasons.
One of them can be an inflammatory process, which we call this Myositis, and then we have to find out what is causing Myositis. But that’s not so common in pain clinics.
Another one can be an injury to the muscle; if there is a hematoma or bleeding inside of the muscle, that can cause severe acute pain.
Myopathies are genetic or hereditary conditions that affect the muscles but are not usually a cause of pain or chronic pain.
It can also be a side effect of medication, for example, some medications used to lower cholesterol.
It can also be the withdrawal of some medications; for example, if a person is using opioids every day and they skip one dose, they may have muscle aches all over their body because that’s a symptom of opioid withdrawal.
Muscle pain can also be radiating from other areas of the body, so if a person has a nerve injury at the level of the spine, we call that radiculopathy, they may have been radiating to the muscles. The problem is not the muscles, but that’s where they feel the pain.
It can also be a deficiency of some vitamins or nutrients, one of them is vitamin D, and it can also be some hormonal problems like problems with the thyroid can also cause some muscle pain.
And finally, there are some chronic infections, such as urinary infections, that are ongoing untreated and can also lead to chronic muscle pain.
However, in pain clinics, the most common types of muscle pain are either fibromyalgia or myofascial pain syndrome.
Found something interesting ?
Get better results by upgrading today!
What's Going On Inside Of The Trigger Point?
The trigger points to a very tiny area of the muscle; what’s going on is that that tiny area is contracted, and there is no blood flow. If there is no blood flow, there is no oxygen. If there is no oxygen, that area cannot relax because the muscle needs oxygen to relax, so it’s squeezing the nerve endings and it’s squeezing the receptors for pain.
There is no blood flow, no oxygen, and it cannot relax by itself, so it’s perpetuating itself.
What are some of the causes of myofascial pain?
It could be repetitive movements, it could be a bad posture, it could be exposed to a cold environment, or it could be other trigger points that are activating trigger points in other muscles. It could be emotional stress; we all carry some stress in our muscles and tense our muscles.
So it can also be because the muscles are weak or short, and when a person tries to use that muscle, the muscle is not ready to be used.
So if a person develops a trigger point in one muscle, what happens is: that muscle will not want to work, will not want to be contacted, will not want to be stretched, and what happens is the muscles around that one will have to work overtime to compensate that muscle that is not working correctly, and then the other muscles around will start having trigger points too.
So the pain starts spreading, that’s very common, that people tell us the pain started here, but now I have pain the whole region here.
So myofascial pain is a region of the body that is hurting, and the pain is diffuse, is difficult to localize, and when we put pressure on those points, we find the pain, the pain that the patient is complaining about.

How do we diagnose myofascial pain?
There is no imaging, no laboratory tests, no blood tests, no electromyography, and no muscle biopsy that can detect the trigger points.
It’s basically with our fingers at this point; the best technique we have is palpating the patient, palpating the whole muscle.
So, finding the taut bands looks like a rope inside the muscle, and inside that taut band, we find the areas of tenderness, and the patient tells us: Wow, that’s my pain! You found my pain doctor! That’s usually how we diagnose.
How do we treat myofascial pain?
So basically, there are two
things we need to do:
1) is to treat what caused myofascial pain, the perpetuating and the precipitating factors, and what’s maintaining the myofascial pain. And the second thing that we need to do is how can we eliminate those trigger points.
For the underlying predisposing factors, we need to see if there is a gait or posture problem if the person is doing any repetitive movement. If there is any joint instability, we need to take some details about what’s going on in the person’s life and why they have that myofascial pain.
Also, in some cases, it can be that there is constant pressure or constriction of the muscles; there can be a tight bra, it can be a purse strap, and it was a heavy purse.
It can also be a tight belt, so anything that is putting pressure on the muscles could be perpetuating myofascial pain. It could also be some nutritional deficiencies the person is not eating a proper diet; the person is deficient in some vitamins, minerals, proteins, folate, and vitamin D, so we need to see if that’s the case for that person.
It can also be some metabolic or hormonal deficiencies, so we need to see if there are thyroid problems, diabetes, or neuropathies. And also, if the person does not have any psychological distress, it’s very common in our society today that anxious people to have a depressed mood.
If we don’t treat the psychological aspect, the person will always carry the stress in their muscles, and it will not get better; they will not get better. Sometimes can also be like a chronic infection. It could be a bladder infection, an intestinal, gastrointestinal, or gastrointestinal infection that we need to treat. It can also be a problem with sleep; the person is not sleeping well or is not sleeping the amount of sleep they require, so we also need to talk about how we will improve their sleep.
Another thing could be a nerve impingement in an area that is then innovating all those muscles.
So if we treat nerve impingement, then the myofascial pain can get much better, and also we need to look at the environment. Is the person working or living in a very cold environment also contracting their muscles?
That can also be perpetuated. So there are many, many things that we need to see what is perpetuating those trigger points because if we don’t treat those conditions, the pain will not go away.
How do we eliminate the trigger points?
There are many techniques we can use to eliminate your points. One thing is true: if we use multi modalities, the elimination will be much faster and more efficient, and if we start treating the myofascial pain right when the myofascial pain started.
If I see patients with myofascial pain for 10, 15, 20, or 30 years, that will be much more complicated. It’s not impossible, but it will be much more complicated.
What are some of the techniques that we use to eliminate trigger points?
The main one will be moving those muscles and doing exercises with those muscles. And for muscle pain, we must think: we need to do four types of exercise.
What are those four types of exercise?
If the muscle with a trigger point is weak, we need to strengthen that muscle, so the first one is the strengthening exercises. Also, if that muscle with a trigger point doesn’t want to be used, the muscle gets shorter.
So we need to stretch the muscle, so that’s the second type of exercise; we need to do stretching exercises. But also, the muscles need oxygen, so we need to pump oxygen to break those trigger points, and how we pump oxygen to our whole body is doing cardio, and aerobic exercise, so that’s the third type of exercise.
And then the last one that many people forget is that we need to relax our muscles, and we need to learn how to do this. That’s the last type of exercise. So we tell our patients to remember the SSAR.
Those are the four types of exercises that we need to do for myofascial pain. Then, we also have many other things we can do to get rid of those trigger points. One of them is the modalities.
We can use modalities such as heat (which can be superficial heat or deep heat). It can also be the application of ice. Some people get better; they get better from the trigger points with applying ice. Although I don’t recommend that much if the person gets better, I am okay with that. Another one can be electrotherapy, the application of electricity: TENS, electrical muscle stimulation that helps the muscle to contract, or the TENS that will help the endorphins of the nerve system to be produced in those are analgesics. It can also be the application of laser, so all of these are what we call modalities.
Another thing is: that we need to relax the muscles. They can also be done with relaxation techniques, biofeedback, and CBT, it can be also helpful for CBT for sleep, and CBT for anxiety, so that’s excellent if the person can relax their mind with cognitive behaviour therapy or any relaxation technique, meditation, or any other breathing exercises, that will relax their muscles.
We can also use manual therapies, such as massage, manipulation, and mobilization, which are great for muscle pain. Then there are also things more invasive, like putting needles on people.
These can be acupuncture in Newmarket, can be dry needling, it can be injections. I do trigger point injections with lidocaine, it’s a local anesthetic, and that’s to help to break that area of the trigger points because the needle will go there and will make the blood flow to wash that area and get rid of all of that contraction.
Treatment of myofascial pain syndrome
- Fibromyalgia is not a disease of the muscle. It’s a disease of the pain system; the person will feel pain all over the body and all the muscles of their body, but that’s because the threshold to feel pain is lower in fibromyalgia, so what a person that doesn’t have fibromyalgia would tolerate a lot of pressure to the muscles without having pain, in fibromyalgia that same pressure will trigger pain, and that’s because the threshold is lower. We need to fix the pain system instead of fixing the muscles. And it’s interesting that exercises, exercising the muscles of the body, all over the body is one of the treatments of the pain system because that will and healthy impulses to the brain and we’ll retrain the brain again how to feel pain normal again. So even though fibromyalgia is not a disease of the muscles, exercising the muscles and moving the muscles is one of the treatments for fibromyalgia.
Treatment of myofascial pain syndrome aims to release trigger points and return the affected muscle to its original length and strength. Standard treatment options include: - Manual therapy, such as massage: manual therapy involves applying a certain amount of pressure to release trigger points. The outcome of manual therapy strongly depends on the therapist’s skill level.
- The Spray and Stretch technique: this technique makes use of a vapour coolant to quickly cool the skin while passively stretching the target muscle. A sudden drop in skin temperature provides a pain relief effect, allowing the muscle to fully stretch and thus releasing the trigger point.
- Trigger point injections with saline, local anesthetics or steroids.
- Dry needling – needle insertion without injecting any solution – is reported to be as effective as injections.





