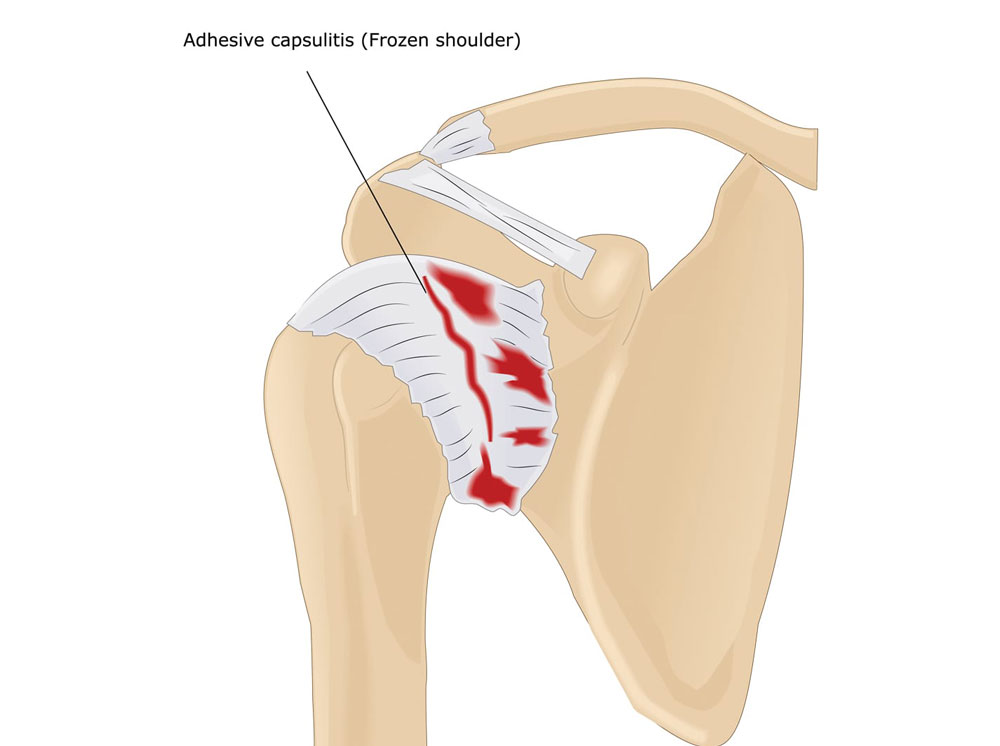
Frozen shoulder, also called adhesive capsulitis, causes pain and stiffness. Over time, the shoulder becomes very hard to move.
Frozen shoulder is a condition that affects your shoulder joint. It usually involves pain and stiffness that develops gradually, worsens, and finally disappears. This can take anywhere from a year to 3 years.
Frozen shoulder is a common disorder that causes pain, stiffness, and loss of normal range of motion in the shoulder. It affects mainly people ages 40 to 60 — women more often than men. The resulting disability can be severe and worsens with time if not treated.
The capsule becomes so thick and tight with a frozen shoulder that it’s hard to move. Bands of scar tissue form, and there’s less of a liquid called synovial fluid to keep the joint lubricated. These things limit motion even more.
Who Gets Frozen Shoulder?
The frozen shoulder risk is increased when you don’t receive exercise therapy after tendinitis or an injury and when you wear a sling for more than a few days without intermittent stretching.
About 10% of people with rotator cuff disorders develop frozen shoulders. Enforced immobility resulting from a stroke, heart condition, or surgery may also result in a frozen shoulder. Other conditions that raise the risk of a frozen shoulder are thyroid disorders and Parkinson’s disease.
How Does a Frozen Shoulder Happen?
The process usually begins with an injury (such as a fracture) or inflammation of the soft tissues, typically due to overuse injuries such as bursitis or tendinitis of the rotator cuff. Inflammation causes worse pain with movement and limits the shoulder’s range of motion.
When the shoulder becomes immobilized, the connective tissue surrounding the glenohumeral joint — the joint capsule — thickens and contracts, losing its average capacity to stretch. Avoiding the pain caused by moving the shoulder leads to further capsule contraction.
The humerus has less space to move in, and the joint may lose its lubricating synovial fluid. In advanced cases, bands of scar tissue (adhesions) form between the joint capsule and the head of the humerus.
Sports-specific injuries can differ from everyday injuries.
How Is Frozen Shoulder Diagnosed?
To diagnose a frozen shoulder, your doctor will:
Discuss your symptoms and review your medical history.
Conduct a physical exam of your arms and shoulders:
The doctor will move your shoulder in all directions to check the range of motion and if there is pain with movement.
This type of exam, in which your doctor is moving your arm and not you, determines your “passive range of motion.”
The doctor will also watch you move your shoulder to see your “active range of motion.”
The two types of motion are compared. People with frozen shoulders have a limited range of active and passive motion.
Advanced imaging tests, such as magnetic resonance imaging (MRI) and ultrasound, are usually unnecessary to diagnose a frozen shoulder.
X-rays of the shoulder are also routinely obtained to ensure the cause of the symptoms is not due to another problem with the shoulder, such as arthritis. They may be taken to look for other issues, such as a rotator cuff tear.

Can Frozen Shoulder be Prevented?
The chance of a frozen shoulder can be prevented or at least lessened if physical therapy is started shortly after any shoulder injury in which shoulder movement is painful or difficult. Your physical therapist can develop an exercise program to meet your specific needs.
How Is Frozen Shoulder Treated?
The two primary goals of treatment are to increase motion and decrease pain. To increase activity, physical therapy is usually prescribed.
The physical therapist moves the patient’s arm to stretch the capsule and teaches the patient home exercises that may include using a wand or overhead pulley. He or she may also use ice, heat, ultrasound or electrical stimulation.
The therapist will demonstrate a stretching program that you should do at least once or twice a day. These exercises include using a cane, a home pulley system and an elastic cord to increase the motion of the shoulder.
Physicians frequently recommend anti-inflammatory medications such as aspirin, ibuprofen (Motrin, Advil), Naprosyn or Aleve to decrease pain. Pain pills such as Tylenol or narcotics may be prescribed to reduce the pain after therapy or help sleep at night.
Occasionally, steroid injections of the joint or the bursa may be indicated. Steroids like prednisone, taken by mouth, may be given to help decrease inflammation.
Stages
Symptoms are usually classified in three stages; they worsen gradually and then resolve within a 2- to 3-year period.
The AAOS describes three stages:
Freezing, or painful stage: Pain increases gradually, making shoulder motion harder and harder. This stage can last from 6 weeks to 9 months. Pain tends to be worse at night.
Frozen: Pain does not worsen and may decrease at this stage. The shoulder remains stiff. It can last 4 to 6 months, and movement may be restricted.
Thawing: Movement gets more accessible and may eventually return to normal. Pain may fade but occasionally recur. This takes between 6 months and two years.
Over 90 percent of people find that simple exercises and pain control improve symptoms. A frozen shoulder recovers typically, but it can take three years.
When Is Surgery Indicated?
Surgery may be indicated if the above program does not improve the range of motion and decrease the pain. After the patient has had a general or regional anesthetic, the physician may manipulate the shoulder in the operating room to break down the scarring.
Occasionally, an arthroscope (a small instrument with an attached camera placed into the shoulder through a small puncture-type incision) is used to cut or release the capsular adhesions directly. Most patients begin physical therapy the same or the following day of the manipulation.
Other operations, such as removing spurs, may also be indicated or required during the manipulation. These operations can sometimes be done with the arthroscope but may require one or two larger incisions around the shoulder (open surgery).





